Elbow Arthroscopy
Information on this article from American Academy of Orthopedic Surgeons
Introduction
The information provided in this website is aimed to provide a general overview of elbow arthroscopy. By no means does this document offer a full comprehensive review of all elbow problems or treatment options. Be sure to discuss your questions with your surgeon. There are significant variations of elbow arthroscopy techniques from surgeon to surgeon.
Overview
Arthroscopy is a procedure that orthopedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word arthroscopy comes from two Greek words, "arthro" (joint) and "skopein" (to look). The term literally means "to look within the joint." During elbow arthroscopy, your surgeon inserts a small camera, called an arthroscope, into your elbow joint. The camera displays pictures on a television screen, and your surgeon uses these images to guide miniature surgical instruments. Because the arthroscope and surgical instruments are thin, your surgeon can use very small incisions (cuts), rather than the larger incision needed for open surgery. This results in less pain for patients, less joint stiffness, and often shortens the time it takes to recover and return to favorite activities.
Elbow arthroscopy has been performed since the 1980s. It has made diagnosis, treatment, and recovery from surgery easier and faster than was once thought possible. Improvements to elbow arthroscopy occur every year as new instruments and techniques are developed.
Anatomy
The elbow is a complex joint formed by the joining of three bones:
- The humerus (upper arm bone)
- The ulna (forearm bone on the pinky finger side)
- The radius (forearm bone on the thumb side)
The surfaces of the bones where they meet to form the elbow joint are covered with articular cartilage, a smooth substance that protects the bones and acts as a natural cushion to absorb forces across the joint. A thin, smooth tissue called synovial membrane covers all remaining surfaces inside the elbow joint. In a healthy elbow, this membrane makes a small amount of fluid that lubricates the cartilage and eliminates almost any friction as you bend and rotate your arm. On the inner and outer sides of the elbow, thicker ligaments (collateral ligaments) hold the elbow joint together and prevent dislocation. The elbow joint is surrounded by muscles on the front and back sides. In addition, the three major nerves that cross the elbow joint are located close to the joint surfaces and capsule and must be protected during arthroscopic surgery.
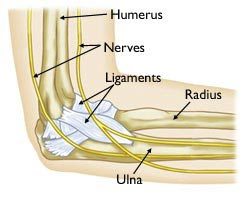
Bones of the elbow joint include the humerus (upper arm bone) and the ulna and radius of the forearm.
The elbow joint allows two basic movements: bending and straightening (flexion and extension) and forearm rotation (pronation — palm down, and supination — palm up).
Normal bending and straightening motion occurs at the joining of the humerus and ulna bones. Forearm rotation occurs at the joining of the ulna and radius and is also influenced by muscles and ligaments further down the forearm and at the wrist joint.
When Is Elbow Arthroscopy Recommended
Your doctor may recommend elbow arthroscopy if you have a painful condition that does not respond to nonsurgical treatment. Nonsurgical treatment includes rest, physical therapy, and medications or injections that can reduce inflammation. Inflammation is one of your body's normal reactions to injury or disease. In an injured or diseased elbow joint, inflammation causes swelling, pain, and stiffness.
Injury, overuse, and age-related wear and tear are responsible for most elbow problems. Elbow arthroscopy may relieve painful symptoms of many problems that damage the cartilage surfaces and other soft tissues surrounding the joint. Elbow arthroscopy may also be recommended to remove loose pieces of bone and cartilage, or release scar tissue that is blocking motion.
Common arthroscopic procedures include:
- Treatment of tennis elbow (lateral epicondylitis)
- Removal of loose bodies (loose cartilage and bone fragments)
- Release of scar tissue to improve range of motion
- Treatment of osteoarthritis (wear and tear arthritis)
- Treatment of rheumatoid arthritis (inflammatory arthritis)
- Treatment of osteochondritis dissecans (activity related damage to the capitellum portion of the humerus seen in throwers or gymnasts)
There are several elbow surgical treatments that are currently most effective when done as an open, traditional procedure. These include surgeries to:
- Treat golfer's elbow (medial epicondylitis)
- Repair the collateral ligaments
- Fix many fractures
- Replace the elbow joint
- Decompress the ulnar nerve (funny bone nerve)
- Some advanced surgeries combine arthroscopic and open procedures in the same setting. For example, in a severe case of osteochondritis dissecans, a loose piece of bone may be removed arthroscopically, and the damaged area of the humerus may be treated with a bone graft using an open surgical technique.
Evaluation & Tests
Your orthopedic surgeon may ask you to see your primary doctor to make sure that you do not have any medical problems that need to be addressed before your surgery. Blood tests, an electrocardiogram, or chest x-ray may be needed to safely perform your surgery.
If you have certain health risks, a more extensive evaluation may be necessary before your surgery. Be sure to inform your orthopaedic surgeon of any medications or supplements that you take. You may need to stop taking some of these prior to surgery.
If you are generally healthy, your arthroscopy will most likely be performed as an outpatient. This means you will not need to stay overnight at the hospital.
Admission & Instructions
The hospital or surgery center will contact you ahead of time to provide specific details about your procedure. Make sure to follow the instructions on when to arrive and especially on when to stop eating or drinking prior to your surgery.
Anesthesia
Before the operation, a member of the anesthesia staff will talk with you about anesthesia options. Elbow arthroscopy is usually performed using general anesthesia, meaning you are put to sleep.
Regional nerve block injections that numb just your elbow area are rarely used in elbow arthroscopy because the numbing effect can last for a few hours after the procedure is completed. Although the numbing effect can help with managing pain, it prevents your surgeon from completing a careful nerve examination in the recovery room to make sure that the nerves that travel down your arm are functioning well.
If necessary for pain control, a regional anesthetic may be provided in the recovery room after your surgeon completes the nerve examination.
Surgical Procedure
Your surgeon will first fill the elbow joint with fluid. The fluid helps your surgeon more clearly see the structures of your elbow through the camera on the arthroscope. This lessens the risk of injury to the blood vessels and nerves surrounding your elbow joint. Your surgeon will make several small incisions to introduce the arthroscope and small instruments into the joint.
Fluid flows through the arthroscope to keep the view clear and control any bleeding. Images from the arthroscope are projected on the video screen showing your surgeon the inside of your elbow and any problems. Your surgeon will evaluate the joint before beginning any specific treatments. If indicated, the entire joint will be evaluated, which may require a total of five or six very small arthroscopy incisions.
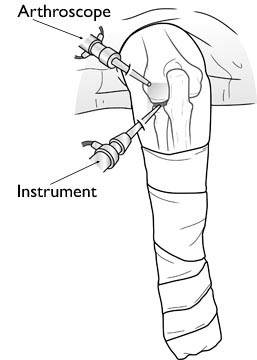
During arthroscopy, your surgeon inserts the arthroscope and small instruments into your elbow joint. Once the problem is clearly identified, your surgeon will insert other small instruments through separate incisions to repair it. Specialized instruments are used for tasks like shaving, cutting, grasping, suture passing, and knot tying. In many cases, special devices are used to anchor stitches into bone. The arthroscopy incisions are usually stitched or covered with skin tapes at the end of the surgery. An absorbent dressing is applied to the elbow. Depending upon the procedure, your surgeon will place either an additional soft dressing that will allow movement or a plaster splint that will restrict movement and better protect the elbow.
Recovery
- Postoperative
After surgery, you will stay in the recovery room for 1 to 2 hours before being discharged home. Nurses will monitor your responsiveness and provide pain medication, if needed. You will be provided discharge instructions that cover medications, need for ice and elevation, as well dressing care. You will need someone to drive you home and stay with you for at least the first night.
- At Home
Although recovery from arthroscopy is often faster than recovery from open surgery, it may still take weeks for your elbow joint to completely recover.
You can expect some pain and discomfort for at least a week after surgery. If you have had a more extensive surgery, however, it may take several weeks before your pain subsides. Your doctor will likely prescribe pain medicine to be taken regularly for the first few days after surgery. In addition, other medicines such as stool softeners or anti-inflammatory medicines may be prescribed.
It is important to ice and elevate your elbow regularly for 48 hours after surgery. This will reduce the risk of severe swelling and help to relieve pain. When elevating your arm, whether you lie flat or recline, make sure your elbow is resting higher than your heart and your hand is positioned higher than your elbow. Depending on the type of surgery performed, your doctor may have specific instructions for longer periods of ice and elevation.
You will most likely be encouraged to move your fingers and wrist frequently to help stimulate circulation and minimize swelling. Your doctor may recommend early range-of-motion exercises to prevent joint stiffness. When you can start these gentle exercises, as well as return to daily activities, will depend on the type of surgery performed.
Dressing care will depend on the type of surgery performed and the preferences of your doctor. In most cases, the operative dressing and/or splint is removed 2 to 3 days after surgery. During this time, your dressing must be left intact and kept dry. In some instances, you may be instructed to keep the dressing in place until your first postoperative clinic visit with your doctor.
- Rehabilitation
Rehabilitation plays an important role in getting you back to your daily activities. An exercise program will help you regain elbow and forearm motion and strength. Your surgeon will develop a rehabilitation plan based on the surgical procedures you required.
In some cases, your doctor will instruct you or a family member with basic exercises to begin at home a few days following surgery. In more advanced surgeries, physical therapy is often prescribed after the first postoperative visit to facilitate motion, strength, and return of function of the elbow. The type and duration of therapy will depend on the type of problem you have and the type of surgery you required.
Return to driving, basic activities of daily living, and return to work will depend on the type of surgery you required and should be discussed with your doctor prior to surgery.
Complications
Most patients do not experience complications from elbow arthroscopy. As with any surgery, however, there are some risks. These are usually minor and treatable and not likely to affect your final outcome. However, most studies do report a slightly higher risk of infection and nerve irritation/injury following elbow arthroscopy as compared to arthroscopy of the shoulder and knee joints. Potential problems with elbow arthroscopy include infection, excessive bleeding, blood clots, and damage to blood vessels or nerves.
Your doctor will discuss the potential risks and benefits of elbow arthroscopy with you prior to surgery. These risks are somewhat dependent on the type of surgery to be performed with the arthroscope.
Long-Term Outcomes
Because patients have varied elbow conditions, complete recovery time is different for everyone.
If you have had a minor repair, you may not need a splint and your range of motion and function may return after a short period of rehabilitation. You may be able to return to work or school within a few days of your procedure.
It takes longer to recover from more complicated procedures. Although the incisions are small in arthroscopy, extensive damage within the joint can be repaired with the procedure. Full recovery may take several months. Although it can be a slow process, following your surgeon's guidelines and rehabilitation plan is vital to a successful outcome.













